
More evidence that low-calorie sweeteners are bad for your health
Studies show that artificial sweeteners can raise the risk of hypertension, metabolic syndrome, type 2 diabetes and heart disease, including stroke.
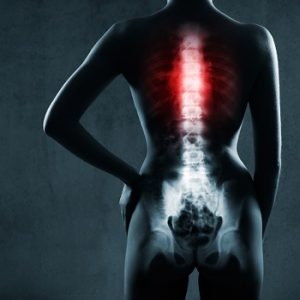
Osteoporosis, which means “porous bones,” is the name for any disease that reduces bone mass.
With age, some bone loss is natural in both women and men, yet it’s only when bones become thin and brittle that the symptoms of osteoporosis occur. These symptoms include leg and foot cramps, loss of height, lower back pain, hip, wrist and spine fractures, and a dowager’s hump (a forward bending of the spine in the upper back).
Women are four times more likely to develop osteoporosis than men. In general, osteoporosis in men is considered a symptom of something else (medication use, lifestyle, diet) while in women it’s almost always a postmenopausal phenomenon.
When women go through menopause, they experience a rapid reduction in bone mineral density, while the decrease is more gradual in men as they age. Women may also be more susceptible than men to osteoporosis because they begin with less bone mass and menopause may accelerate the process of loss. In both ageing women and men, the acceleration of bone loss is caused by drops in the production of estrogen and testosterone.
The good news is that there are many things that you can do to promote and maintain strong healthy bones
Choose dietary sources of calcium carefully
When most of us think of building strong bones we think of calcium (and dairy products). But while calcium may help, even the most positive trials show that calcium on its own is not enough. In addition, as a general rule, countries that have the highest traditional consumption of dairy products (United States, Sweden, Israel, Finland, and the United Kingdom) also have the highest rates of osteoporosis-related hip fractures.
This may be in part because different dairy products appear to have different effects on bone density and fracture rates. Milk, especially nonfat milk, is a good choice because it is relatively low in protein and salt, and higher in calcium. Cottage cheese and some hard cheeses, however, can be high in protein and salt and potassium (which can accelerate the removal of calcium from the body) and low in calcium.
Although there may be better ways of getting calcium (such as dark green vegetables), younger women may benefit over the long run from including some nonfat milk and nonfat yogurt in their diets.
Getting enough calcium from your diet is likely to build stronger bones than if you are taking supplements. In addition, high dose supplements may have adverse effects on health.
Watch vitamin D levels
Vitamin D plays an important role in protecting your bones by helping your bones to absorb calcium. Adults age 50 and older need 800 – 1,000 IU of vitamin D every day. Some people may need more and it’s worth having your levels properly assessed in order to devise an optimal supplementation programme that meets your individual needs.
Look at your diet holistically
The disproportionate focus on calcium as the most important bone builder means that many women and men at risk from osteoporosis miss out on other equally important nutrients. Because of this it’s worth looking at your diet and considering whether you are getting enough of these other bone building co-factors:
Zinc, Manganese and copper levels in people with osteoporosis are often low too. Including more dark green and leafy vegetables and brassicas (broccoli, cabbage, Brussels sprouts etc) in your diet can go a long way towards boosting your intake of most of these nutrients.
Cut out the caffeine
Caffeine increases urinary loss of calcium and has long been linked to increased risk of hip fractures and to a lower bone density especially in women. Curiously, while consumption of caffeine-containing tea has been linked to osteoporosis in some studies, others have reported that tea drinkers have a lower risk of osteoporosis than do people who do not drink tea.
It is possible that the calcium-excreting effect of caffeine in tea may be compensated for by other constituents such as antioxidants. In particular laboratory studies show that the flavonoids in green tea may help increases in bone mineral density.
In the same vein early studies found that regular intake of carbonated sodas seemed to reduce bone mineral density. It was thought that phosphoric acid, added to sodas to give them ‘bite’ was responsible. Subsequent studies however have shown that colas (as opposed to fruit based sodas) are the most damaging (again more for women than men) and this is likely because of their caffeine content.
Protein: enough is as good as a feast
Protein has a paradoxical effect on bones. On one hand, it increases the loss of calcium in urine, which should increase the risk of osteoporosis. On the other, normal bone formation requires adequate dietary protein, and low dietary protein intake has been associated with low bone mineral density.
Unfortunately the line between too much protein and too little protein remains elusive. In the West many of us take in more than we need which has other implications for health and can place a strain on the kidneys. The key it seems is moderation in all things; 60- 90 g (2-3 oz) of meat or its plant equivalent per day is adequate protein for most of us.
Good oils
Diets rich in the omega-3s from oily fish or algae (DHA and EPA), which also naturally result in a more favourable ratio of omega-6 to omega-3 fats, appear to reduce bone loss. In a recent study 1200 mg daily of omega 3 combined with aerobic exercise raised bone mineral density in women by 19%.
While the bulk of studies focus on the use of fish oil there are good reasons both environmental and nutritionally to consider plant sources; fish are a rapidly dwindling resource and it is impossible to tell if a fish – and its oil – has been contaminated with toxins that get dumped in our seas. Evidence suggests that plant sources of omega 3s are protective and may help reduce inflammation associated with osteoporosis. The polyphenols in olive oil have also been found to be protective.
Exercise benefits in two ways
Load bearing exercises help to keep your bones strong and increases muscle mass, which in turn helps strengthen bones. Aim for at least 20-60 minutes, three times a week, with an activity you enjoy. Good choices include walking, aerobics, jogging, weights, racquet sports, cycling etc.
Protect your adrenals
Your adrenal glands go on producing a useful form of estrogen after menopause. This may help to keep bones strong. Wherever possible investigate lowering stress (see our article De-stress, Naturally) while practising the other advice on this page.
Put that cigarette out!
Cigarette smoking was first identified as a risk factor for osteoporosis more than 20 years ago. Recent studies have shown a direct relationship between tobacco use and decreased bone density in both men and women.
Maintain a sensible weight
Yo-yo, crash and fad dieting are poor ways to lose weight over the longer term and they may cause bone loss which is difficult to remedy. Aim for sensible weight loss programmes and a steady weight. After the age of 50 carrying a little extra weight may even help protect bones in women, while maintain good muscle mass is protective for men.
Cut back on salt
Although a definitive link between salt intake and osteoporosis has not yet been proven, many doctors recommend that people wishing to protect themselves against bone loss use less salt and eat fewer processed and restaurant foods, which tend to be highly salted.

Please subscribe me to your newsletter mailing list. I have read the
privacy statement